Since March we’ve all seen an explosion of articles, forum posts, and products regarding aerosols and aerosol risks. The initial pandemic response in the dental and wider medical associations was a fairly predictable one: stay cautious and double down on PPE.
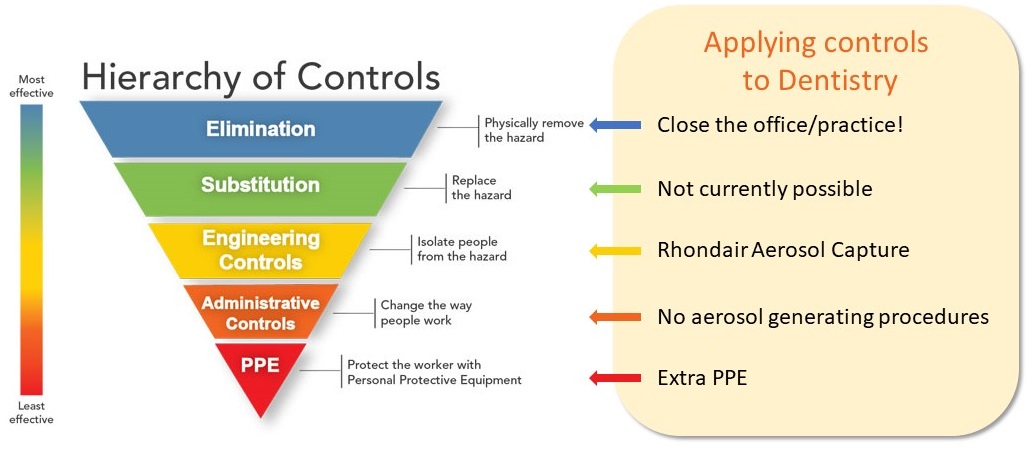
While PPE should absolutely be used, standard health and safety practice dictates that PPE is the least effective hazard control available. PPE should always be the last line of defence, not the first – and certainly not the only one.
Research focuses are now shifting from the immediate “firefighting” nature of choosing what PPE is the most effective, and moving to the wider controls available.
The “Hierarchy of Controls” is based on established safety protocols from The National Institute for Occupational Safety and Health (NIOSH), part of the US Centers for Disease Control and Prevention (CDC). “Engineering controls” – like the Rhondair Aerosol Capture System – isolate people from the hazard and form part of the best risk management strategies available today.
Dispelling Myths
An unfortunate aspect of a pandemic in the information age is the difficulty in discerning misinformation from fact. While this isn’t just a dentistry issue, dentistry is far from protected from it either.
It’s human nature to seek out surety, but of course that was one of the first things to disappear back in the distant past of earlier this year. Everyone is looking for a definitive answer or path forward, but unfortunately there just hasn’t been enough time for all the ideal research and studies to be completed yet.
UV Lights to Kill Viruses?
What we can do though, is approach things with a scientific mindset. For example, the use of UV lights in aerosol capture units. It’s well established that enough ultraviolet light can kill viruses. Therefore, you’d think incorporating UV lights into an Aerosol Capture System would make sense. Well, not really. The problem is one of physics.
To effectively kill a virus with UV light, you need at minimum several seconds of direct UVC light. As aerosols travel through a capture unit they’ll diffuse randomly, meaning there’s almost a zero percent chance that they’ll end up obligingly sitting in place in a duct or on the outermost layer of a filter for long enough to be destroyed.
The US Food and Drug Administration urges caution also:
“It is important to recognize that, generally, UVC cannot inactivate a virus or bacterium if it is not directly exposed to UVC. In other words, the virus or bacterium will not be inactivated if it is covered by dust or soil, embedded in porous surface or on the underside of a surface.”
So while a UV light might make you feel safer, in most instances it’s only a placebo.
HEPA Filters, NASA, and Microns
Another misconception relates to HEPA filters. Many publications, news agencies, and even some suppliers incorrectly state that HEPA filters are only effective down to 0.3 microns.
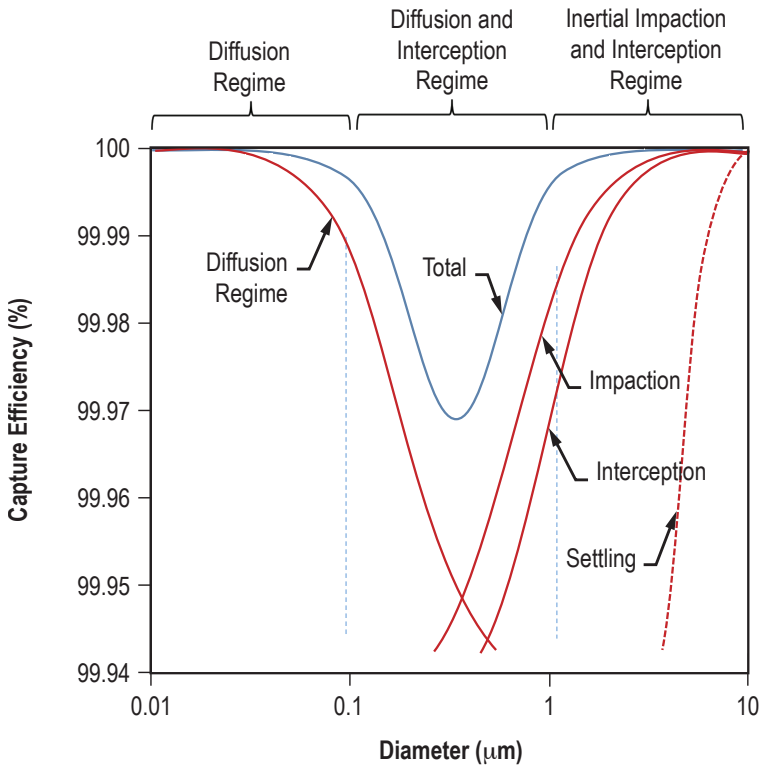
Initially it makes sense; a filter captures particles above a certain size, with anything smaller passing through. However, NASA themselves tested HEPA filters in 2016 and confirmed that they are incredibly effective at capturing particles of all sizes, including below 0.3 microns, to near 100% effectiveness.
Again, the answer lies in some unusual physics, specifically how particles below 0.3 microns behave; a natural phenomenon known as Brownian Motion. When particles are small enough, their movement becomes affected by the individual atoms and molecules around them, including water molecules or the very air itself. These particles move in a random pattern, effectively ricocheting off other matter. Inside a HEPA filter, these particles bounce around and are caught in almost all instances by the multitude of HEPA filter fibres.
When a HEPA filter states its effectiveness, that is actually the lowest rate of its efficiency. At other sizes above and below 0.3 microns, an H13 HEPA filter captures greater than 99.95% of particles.
Although individual COVID-19 viruses are very small (nano-sized), they are only emitted into the atmosphere inside droplets that are much larger (>1 micron). These droplets can contain between 100 and 1,000 viruses. This means that the HEPA filter only needs to catch the droplets, which is much easier since they are in the micron range.
Caveat Emptor
Two little words: “Caveat emptor”. For those of us who don’t happen to speak Latin, this translates to “Let the buyer beware”. It’s commonly seen in contract and consumer law and it’s no less relevant now than when it was first written.
Aerosol capture is a rapidly expanding market for obvious reasons, but if a website or supplier is only showing 3D renders instead of actual physical devices, isn’t showing any customer testimonials, or you see suspiciously similar-looking devices from several different companies, they may all be signs that a product might not be quite as developed as you’d like.
Encouragingly though, dentistry has adapted to widespread changes several times before. Not that long ago the use of gloves wasn’t considered standard either, but I doubt many of us would practice today without them. Not to mention the looks you’d get from a patient if you tried.
Dentistry as an industry will soon have to make a choice about how to move forward; adapt to a new environment or continue with the ambulance at the bottom of the cliff that is PPE alone.
After all, doing nothing is still making a choice.
As always, stay safe.
The team at Rhondium.